I’ve probably spent too much time contemplating if and how
to share my cancer story. Should I write
an inspirational story feigning strength and bravery? Should I simply present the clinical facts? The truth is, I survived because my cancer
was caught early… many people aren’t as fortunate and I’m not comfortable
celebrating my good fortune when I know so many who have had less positive
outcomes. So instead, I’m going to share
the day-to-day reality of a cancer patient because my story would be nothing
more than a few pages of useless words if it didn’t offer some insight that
might be helpful to someone else facing a cancer diagnosis of their own, or of
a friend or loved one.
I remember once asking my doctor what an abnormal breast lump felt like. She commented that benign breast fibroids, cysts, and calcifications are common, but that I had unusually smooth breast tissue – which was good because it would be especially easy for me to notice any changes. She was right. In late 2020, I felt a lump in my breast. However, I assumed it was just changes related to age and with the hassles of appointments during the pandemic, I waited a month or two before calling to schedule that mammogram I was overdue for. I didn’t really want to tell anyone that I felt a lump, I just wanted to know if it showed up on a mammogram. Unfortunately, there was about a 3 month wait for screening mammograms, so on December 15, I saw my primary care provider who scheduled me for a diagnostic mammogram 3 days later.
On December 16, I closed on the purchase of a new home.
More on that later…
The mammogram was followed by an ultrasound – as is always the case for me. Apparently even “smooth” breast tissue can be too dense for a decent quality mammogram image. They found six or seven abnormal spots, so they scheduled me to have them biopsied on Christmas Eve.
This was my first mistake… we have our benefits open enrollment in November, and at that time, I realized that I didn’t use any of my health savings account in 2020. I had more than my annual out of pocket maximum saved, so I reduced the amount I would contribute in 2021. But in the last two weeks of December, I met my full deductible for the year. Had I believed that the biopsies might actually result in a cancer diagnosis, I would have waited 8 days and had them done in the new plan year. That little mistake cost several thousand dollars, as the tests and surgeries scheduled in January quickly added up to my deductible for 2021.
Although my clinic didn’t allow guests to accompany patients to appointments during the pandemic, they made an exception and Jim was allowed to sit beside me during the biopsies on Christmas Eve. They took over 20 tissue samples from 6 different sites. Only one of the sites was the lump I could feel. There was one more spot that they wanted to sample, but I was nearing the limit for how much lidocaine they could inject in me in a day, so we decided to wait until we got the results before taking any more. I remember not wanting to worry my family on Christmas Eve, so I stuffed ice packs in my bra on the drive to dinner at my sister’s house, then hung them from the passenger side window of my SUV while we ate so they would re-freeze for the ride home. My brother-in-law doesn’t miss a thing, so of course he asked what was hanging from my car door – I don’t recall the answer I gave, I think I just tried to quickly change the subject.
There was a lot of waiting due to the holidays. Sometime around January 8, 2021, I learned that the biopsies revealed a 2.3 cm ductal carcinoma in situ (DCIS, stage 0) that was positive for both estrogen and progesterone receptors, as well as a rare but benign tubular adenoma, and several fibrous spots that weren’t concerning. Interestingly, many doctors don’t believe that DCIS is palpable, but I confirmed that the DCIS was found in the lump I could feel. Treatment for DCIS is typically partial mastectomy (lumpectomy) followed by radiation treatment. However, my oncologist recommended more testing before making a final decision on the treatment approach.
A quick note on DCIS. It is not invasive and is considered Stage 0. Some people consider it “pre-cancerous”, but it can become an invasive cancer if left untreated. I know someone who had this diagnosis and was told she didn’t have “real” cancer because she didn’t need chemotherapy and didn’t lose her hair. As far as breast cancer diagnoses go, it is the best one to get in terms of outcome, but it is still a cancer diagnosis! Please don’t ever downplay what someone is going through during cancer treatment just because the staging is low, or their prognosis is excellent. Cancer treatment sucks, even when the cancer itself isn’t one of the “bad ones”.
A breast MRI and genetics study were added to the list of tests to undergo before deciding on a treatment plan. While waiting for the genetic test results (which came back negative for any gene mutations that made recurrence more likely), Jim and I began moving our belongings from both of our apartments into the new house. I was on a lifting restriction for part of this, so things went much slower than I had planned. We got everything into the garage and set up the bare necessities in time for my lumpectomy on February 18th. The surgery went smoothly, although I was a bit unsettled when one of the meds given to me immediately before the surgery caused a loud ringing in my ears. I woke from surgery more easily than I usually do with no noticeable side effects from the anesthesia, so I went home and logged into work.
Prior to my surgery, I hadn’t told anyone about the diagnosis except for immediate family and two close friends. I posted about my experience on social media the evening of my surgery, which likely caused several other close friends to wonder why I hadn’t told them. The truth is, I didn’t want to worry people before I had answers. At that point, I thought I was done with everything except a few rounds of radiation.
My son’s lease was up at the end of February and so we started adding yet a third household of furnishings to the new house. My phone rang as I was driving a U-Haul truck down Grand Ave in Wausau. It was my oncologist’s nurse wanting to follow-up now that they had the histological results from my lumpectomy. Expecting to be told that everything looked good, I asked if she could call me back in five minutes when I arrived at my son’s apartment. She called again with my oncologist standing by as I stood in my son’s doorway greeting the movers. My phone was acting up, so I answered the call on my watch. Between the background noise of the movers, the low volume of the speaker on my watch, and my oncologist’s heavy accent, I made out only some of what he was telling me before I heard him suggest that I just come to his office.
Upon settling into my oncologist’s office, he explained that they didn’t get clear margins on the lump that was removed, and within that lump were 8 separate cribriform carcinoma tumors that hadn’t been picked up by any of the prior tests. Had there been one tumor the size of the sum of the 8 tumors, it would have been considered a Stage 2 diagnosis. However, technically, I had 8 stage 1 tumors. My oncologist had never seen a case like this, and if the 8 tumors didn’t show up on the tests, it begged the question of whether there were more. Because of this, he recommended we treat it as Stage 2 cancer with chemotherapy and radiation. But first, I had a full body PET scan to look for signs of any other masses, a second surgery to remove more of the area where the first (DCIS) tumor was as well as to remove a couple lymph nodes and insert the port that my chemotherapy would be administered through, followed by a poorly timed echocardiogram less than 24 hours after surgery to make sure my heart could handle chemotherapy.
I remember going into the second surgery on March 4th ready for the loud ringing in my ears again, which didn’t happen, and expecting to wake up feeling as good as I did the last time, which also didn’t happen. I found it curious how the exact same surgery, surgeon, anesthesiologist, and surgical team resulted in two very different experiences. I realized later that day that it was exactly 8 years to the day after I had my right adrenal gland removed due to a tumor that was producing too much aldosterone. Although that tumor wasn’t cancer, I was treated in Froedtert’s Cancer Center. I remember thinking how much nicer Froedtert’s facilities were.
On March 9th, we picked up a new member of my care team…. Sookie, an 8 week old English Springer Spaniel.
I had been given an overwhelming amount of information about my diagnosis, even a book from the hospital where the nurse had marked pages and highlighted parts that were relevant for me. Being who I am, of course I read everything I could get my hands on from reliable sources about the chemotherapy drugs I was told I would receive. On March 10th, I arrived for my first round of chemo and learned they changed which drugs I would receive. I went from planning to have 6 rounds of cyclophosphamide and doxorubicin over a 12 week period to 4 rounds of cyclophosphamide and Taxotere over the same period. Because of the change, I wasn’t familiar with Taxotere but I learned a week later that it is associated with permanent hair loss in some patients.
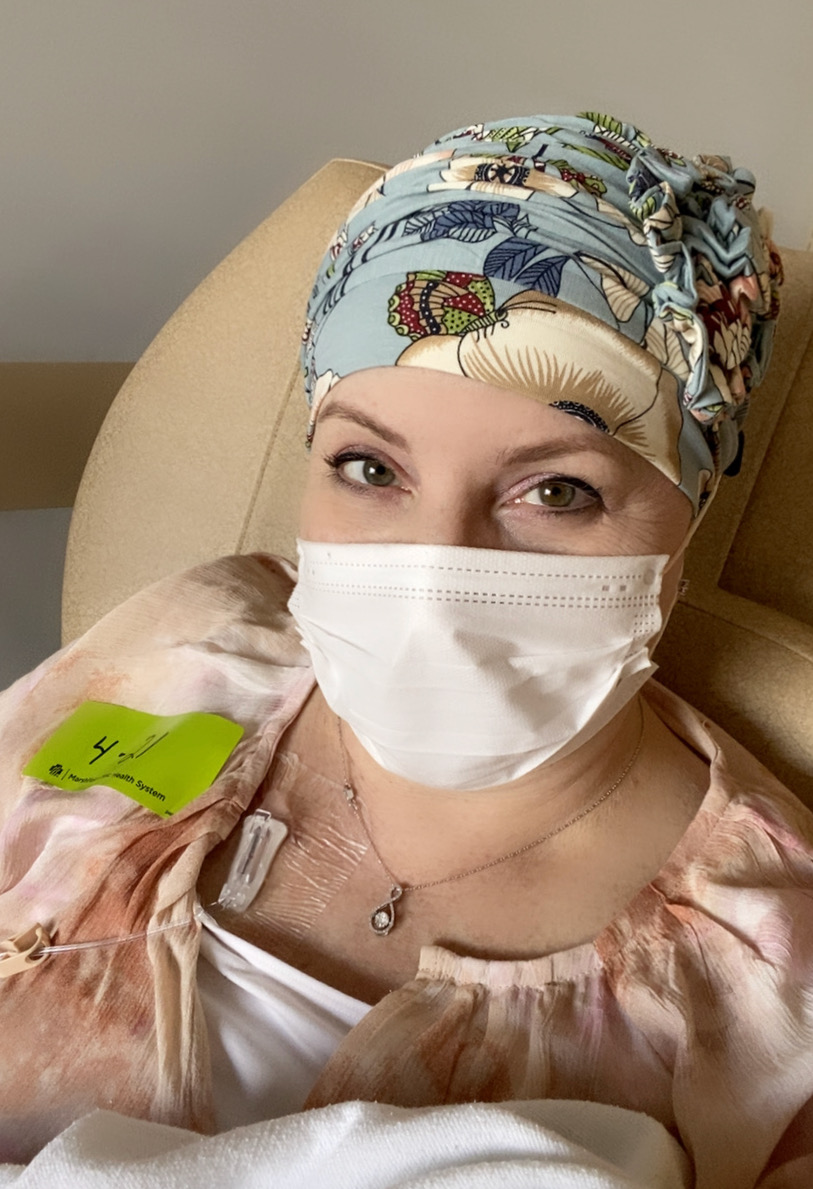
The actual administration of chemotherapy itself isn’t all that bad. I went in early every third Wednesday, from March 10 through May 12. They checked my blood first to make sure I was healthy enough to get the treatment. Then, I relaxed in a chair and was given drugs to prevent nausea as well as a steroid and Benadryl to prevent any reactions to the chemo drugs. I found myself fighting to stay awake long enough for them to start the first chemo drug. All of this, from the blood draw to the drug administration, was done through a needle that was inserted through my skin into the port in my chest. Before sending me home with more pills for nausea, they taped a small device onto the back of my arm which inserted a small tube through my skin. 24 hours later, a dose of Neulasta was injected through that tube, and roughly 20 hours later is when I started to feel like crap. Neulasta is a $6500 shot in the arm that kicks your immune system into high gear, causing your body to rapidly produce white blood cells to prevent infection. In the process of doing this, it causes inflammation in your bone marrow – literally causing every bone in your body to hurt. Badly. I feel nauseous just remembering it.
The weekend after chemo was usually the worst, and that sometimes carried over into Monday, but by Monday evening I was through the worst of it. The thing to remember about chemo, though, is that the effects are cumulative. On March 18th, my best friend flew in from Arizona to spend a few days with me and help me cut the hair that I was about to lose into a short style.
It wasn’t long after that I got tired of shedding and just shaved it all off. I stuck with turbans throughout the chemotherapy and waited until I was feeling better before buying a wig.
As I mentioned, the effects of chemotherapy are cumulative. Although my last treatment was in May, my
blood tests in June still showed my red blood cell count, hemoglobin, hematocrit,
and lymphocyte counts all below the target range. At some point in there, I felt so weak that I
was nervous just taking the one step down into my sunken living room. I can remember carrying a basket of laundry
from my bedroom to the laundry room and just sitting on the floor in tears
because of how hard it was. I felt as if
all my muscles had shrunk. I couldn’t
bend down to pick something up or roll over in bed without feeling like I was
pulling something.
I was spending more time in bed, eating comfort foods to combat the nausea, retaining water, and unable to get comfortable. I felt like a short, bald, fat circus freak. My house was a disaster from the incomplete move, my garage too full of boxes to park in, but I turned down offers of help because I just didn’t want to be seen. At some point during that time, I remember thinking, “If it comes back, I won’t put myself through this again.” Weeks after my last chemo, I was still developing new side effects – my skin started flaking, my nails became discolored and started to lift off, and the edema in my legs became worse. I developed an allergic reaction which presented as a rash across my entire back. That also had to be biopsied to confirm the cause.
I started radiation a week after chemotherapy ended. I was given the option to heal a bit more first, but I had hopes of being done by the 4th of July and maybe being able to enjoy the summer. Every weekday for 4 ½ weeks, the left side of my chest was irradiated. Like the chemo, radiation side effects are cumulative. They also are delayed by about 10 days after the treatment. Although I finished my radiation treatments in mid-June, my skin was still falling off in chunks two weeks later. But at the same time, I also figured out how to wear a wig.
There is more... the estrogen blocking medication that gave me daily migraines, not being able to wear regular antiperspirant or a bra during radiation treatments, trying to find shoes to fit my swollen feet before a business trip, new kidney stone attacks, neuropathy in my feet, continued numbness in my chest and underarm, and so on. But I think the important stuff has been sufficiently covered.
All this might seem like TMI, but I’m sharing the details because inevitably someone would say something like, “Now that you’re done with cancer treatments….” And it is important to realize, being “done” with the treatment is not even close to the same thing as being “done” with the side effects. I’m writing this in mid-Sept, still fighting a rash, as well as some fatigue and weakness. But, I’m still here to share my story, so I guess that makes it all worth it. As for those earlier thoughts that plagued me… In hindsight, yes, I would go through it again if I had to. But I’ve learned a lot… I would do things differently, which means I have to change things now if I want to be prepared for the possibility of a recurrence. There may never be a “next time”, but if there is:
I need to be healthier going into it
My life needs to simpler, my surroundings less overwhelming and chaotic
I must have a fallback plan if I suddenly can’t work, because my health and life insurance are provided by my employer
I need to let go of the things that no longer bring me joy – because hard times will come, but living a life of joy is what allows you to face them without regrets
So that is my story. People comment on how strong I must be to fight cancer, but honestly, there is little bravery in doing what you’re told you must do to stay alive. The one thing I can do by choice for no other reason than because it feels like the right thing to do is to implore you to do the following:
Stay on top of your regular screening exams.
Don’t tell someone who has a health change or concern that it is probably nothing.
Keep more money than you think you need in your HSA, especially if you can carry it over from one year to the next.
Have good health insurance, even if just for major medical conditions - so far, my medical bills have totaled over $300,000.
Don’t minimize a cancer diagnosis because it is early stage or doesn’t require chemotherapy.
Be aware that a cancer patient may feel as obligated to comfort his or her loved ones about the diagnosis as you feel obligated to comfort him or her.
Know that the effects of cancer treatments last much longer than the actual treatment schedule.
If you care for someone facing a cancer diagnosis, understand that the kind of support they need may be completely different than what you think.
If you know someone facing a cancer diagnosis, ask them how they are. Please don’t ask them what their prognosis is, and please don’t be completely absent. Reach out – even if you aren’t sure what to say, trust me, they will notice your silence far more than any awkwardness in your call, email, or text.
Hug your people and tell them you love them because life is short.
Enjoy your life today, tomorrow isn’t guaranteed.









Beautifully written. Thank you for sharing. Sandy
ReplyDeleteWell done. This is helpful for so many people. Thank you. Love and hugs to you, Jim and your family
ReplyDeleteLeslie, I remember the day I first met you. I think you were 6. I'm sorry you're having to go through all this. Thank you for sharing your story; I havea friend currently receiving treatments (over a year already). This helps me understand some of what she's going through. I will keep you in my prayers.
ReplyDelete